Research Article
Volume 5 Issue 1 - 2023
Evaluation of Visual Acuity following Cuban Treatment for Retinitis Pigmentosa.
International Retinitis Pigmentosa Center, Camilo Cienfuegos International Clinic, Havana, Cuba
*Corresponding Author: Dr. Lázaro Joaquín Pérez Aguiar, First and Second Degree Specialist in Ophthalmology, Doctor in Medical Sciences, Professor and Director of Camilo Cienfuegos International Clinic, Havana, Cuba.
Received: January 18, 2023; Published: February 01, 2023
Summary
Objective: Toevaluate the behavior of visual acuity after the application of the Cuban treatment for retinitis pigmentosa.
Methods: Study of 16 patients with retinitis pigmentosa, Snellen 1.0 in both eyes, who underwent Cuban treatment for the disease for 20 years, grouped into four groups according to the frequency of the treatments performed.
Results: In group No.1, treated twice a year, the decrease began 15 years after the first treatment, with five of the eyes studied showing 0.8. At 20 years, six eyes showed 0.8 and two showed 1.0.
In group No. 2, treated once a year, a decrease started 10 years after the first treatment, where nine eyes dropped to 0.8 and one to 0.6. At 20 years four eyes showed 0.8, and six reached 0.6. In groups 3 and 4 the decrease was significant.
Conclusions: Cuban treatment for retinitis pigmentosa achieves better visual acuity control if performed every 6 months. Annual treatments should be evaluated individually to achieve adequate control. Control is not achieved if applied irregularly.
Keywords: Retinitis pigmentosa; Cuban treatment
Introduction
The term retinitis pigmentosa or retinitis pigmentosa (RP) currently groups together a large number of very heterogeneous retinochoroidal diseases with variable forms of inheritance, in which different processes of negative plasticity develop in their pathophysiology, consolidated in a single term, retinal remodeling [1].
Retinal remodeling is a complex process that involves multiple mechanisms such as hypertrophy of Müller cells, metabolic dysregulation, development of aberrant circuits that alter normal retinal circuits, with formation of new axons and new synapses, which generates a reprogramming of all neuronal circuits, alteration of all retinal layers, death of all types of neurons including those of inner layers, modifying the signal processing network [2,3], progressing towards a neurodegenerative process that alters structural and functional proteins recently named proteinopathies [4].
In the fight that science worldwide is currently waging against RP, different therapeutic alternatives have been introduced to try to develop some degree of artificial vision, especially for blind people, such as bionic implants in different retinal layers [5], chips with state-of-the-art materials, including nanotechnology [6,7], stem cells [8,9] and ocular gene therapy [10].
The results achieved so far with these technologies are very limited, because scientists have not taken into account the serious alterations that occur throughout the retinal structure, which prevent the development of useful vision in people blinded by the disease.
Currently, science stimulates the integration of all scientific knowledge to develop multitherapeutic alternatives to combat this incapacitating disease with greater logic, protecting the cell groups that resist and survive the retinal remodeling process, trying to prolong as long as possible the visual function of patients suffering from RP [11].
The Cuban multitherapeutic treatment to treat patients with RP is an integrative strategy of current scientific knowledge, which is divided into two different stages.
The first stage includes an ophthalmologic microsurgery, which applies the retro-orbital fatty tissue on the suprachoroidal space, combined with the application of ozone therapy, electro stimulation and supplements used internationally to combat this disease, with a duration of 21 days. The second stage is the control and follow-up treatment of the disease, which includes a personalized ophthalmologic evaluation and treatment, where ozone therapy, electro-stimulation, magnetotherapy and supplements are applied, lasting 14 days [12,13].
The evaluation of visual acuity in patients who underwent treatment at an early stage is the most important objective of this research, allowing an assessment of their long-term behavior, contributing to enrich the criticism on the possible results to be achieved with the application of this Cuban therapeutic alternative.
Method
A descriptive, longitudinal, retrospective study was carried out on patients with retinitis pigmentosa treated with the Cuban treatment alternative for 20 years at the Camilo Cienfuegos International Clinic.
The study universe consisted of 12,283 patients with RP, diagnosed and treated with the Cuban multitherapeutic treatment for the first time. The inclusion criteria to determine the sample were patients with typical RP (rod-cone degeneration type), Snellen visual acuity 1.0 in both eyes, under 21 years of age at the beginning of treatment. Patients with general diseases and other ophthalmologic diseases were excluded, for which the necessary clinical and ophthalmologic examinations were performed. The international parameter of variation of two Snellen lines in visual acuity was considered for evaluation.
The selected patients were initially submitted to a treatment scheme called RP-1, consisting of an ophthalmologic microsurgery called revitalizing microsurgery (CRV), where a pedicled autologous transposition of retrorbital fatty tissue is performed by applying it on the suprachoroidal space. The following day continues with a session of ozone therapy by rectal insufflation, followed by electrostimulation on the recommended reflexology points using Scy fix 600 equipment. Both therapies are applied once a day for 14 days. Nutritional supplements and eye protection with sun filters are part of the general recommendations at discharge.
The control and follow-up scheme is called RP-2 and consists of a daily session of ozone therapy by rectal insufflation, followed by electrostimulation of the reflexology points using Scy fix 600 equipment for 10 days, with similar general recommendations at discharge.
The final sample consisted of 16 patients who met the inclusion criteria. Of these, 4 patients were able to comply with the control and follow-up schemes every 6 months after PR-1 and were grouped in group No.1. Group No.2 is made up of 5 patients who after PR-1 were able to comply with the control and follow-up schemes (PR-2) once a year. Group No. 3 is made up of 4 patients who, for various reasons, irregularly completed the PR-2 and group No. 4 is made up of 3 patients who completed PR-1 and returned, one at 7 years, the second at 11 years and the third at 19 years.
The study was conducted in compliance with the bioethical principles set forth in Law No. 41 of Public Health, the Declaration of Helsinki and the fundamental premise of informed consent and information on the procedures to be performed on the subjects. The data were collected from the corresponding clinical histories, creating a database in EXCEL of the WINDOWS 10 operating system and the SPSS version 22.0 statistical package where the follow-up of the patients was recorded. In all statistical tests, a reliability level of 95%, statistical significance level of 0.05 was considered.
Results
Snellen visual acuity was evaluated in the 32 eyes of the 16 patients studied. Of them 4 patients are in the group that received treatment twice a year, 5 patients are in the group that performed annual control, another 4 patients in the group that performed the first RP-2 with interval between 3 and 5 years after RP-1 and 3 patients who came the first time and returned at 7, 11 and 19 years respectively from RP-1.
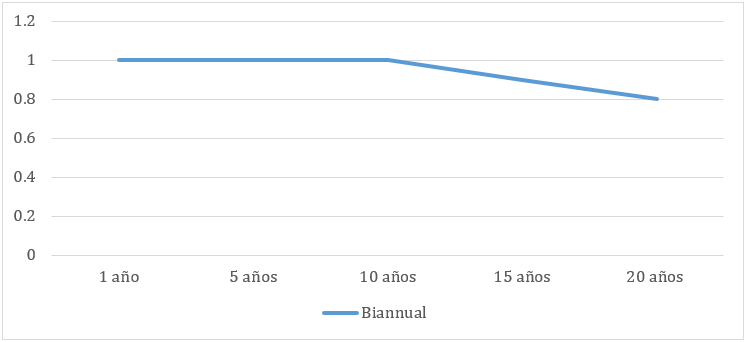
In group No. 1 of 8 eyes with RP-2 twice a year the trend to a decrease in mean VA began 15 years after RP-1, with five eyes studied going to 0.8. The rest (three) maintained 1.0.
At 20 years of age, six eyes showed 0.8 and two showed 1.0, as shown in Graph No. 1:
In group No. 2, which consisted of 10 eyes with annual RP-2, there was a trend towards a decrease in the average VA at 9 years after RP-1. In this group eight eyes showed 0.8 visual acuity at 10 years and two maintained 1.0. At 15 years nine eyes showed 0.8, and one showed 0.6. At 20 years two eyes showed 0.8, and ten eyes showed 0.6.
In group No. 3 consisting of 8 eyes of the 4 patients with RP-2 between 3 and 5 years after RP-1, VA shows four eyes at 0.8 and four others at 0.6 in the first control. At 10 years post RP-1, two of the eyes studied showed 0.6, six others showed a range between 0.5 and 0.4 visual acuity. At 15 years two eyes showed 0.6, and the rest were in the range of 0.5 to 0.3 vision. At 20 years of age one eye was 0.5, and the rest were between 0.4 and 0.2. The trend is shown in graph No. 3.
In group No. 4, which consisted of 3 patients, one returned to his first RP-2 at 7 years of age and his two eyes showed a drop in VA OD of 0.6 and OI of 0.5. The second patient returned at 11 years of age for his first RP-2 and showed OD 0.1 and OI 0.3. The third patient returned at 19 years of age for his first RP-2 and showed OD 00.5 and OI 00.8.
Graph No. 4 compares the evolution observed in the different groups of patients studied.
Discussion
When comparing the evolution of the different treated groups, a lower deterioration of visual acuity was observed in patients who underwent the control and follow-up of the disease (RP-2) every six months, with an average decrease in visual acuity of two Snellen lines, considering this as a positive result for the quality of life of people suffering from this disease, when comparing this group with the natural evolution of the disease, where periods of plateaus and abysses of vision loss are part of the natural history [14].
Among the patients in group No. 2 who underwent RP-2 once a year, differences in VA behavior were observed, with loss of 2 Snellen lines earlier compared to those who underwent it every six months in group No. 1. This result could be influenced by the temporary biological effects of ozone therapy estimated between six to eight months after the previous treatment, and of electrostimulation, which could generate instability at the cellular level that does not ensure adequate control during the remaining months until the next treatment. In group No. 3, which underwent RP-2 between 3 and 5 years after RP-1, the differences are significant in relation to the two previous groups. In group No. 1 the visual stability plateau is prolonged by joining the treatments at the appropriate time, which prevents the sudden loss of visual function. In group No. 2 the abrupt loss was reversed, achieving another level of plateau in a lower step than the previous one, but in group No. 3 the abysses of visual loss was not completely reversed. Group No. 4 shows unfavorable evolutionary results of this parameter under study, and it is not possible to modify the natural history of the disease in each individual.
It is evident that an early diagnosis of the disease and the performance of this therapeutic alternative in the best visual conditions, in regular treatment cycles for the control and follow-up of the disease is the most appropriate. It is also evidenced that patients who underwent control and follow-up treatment every 6 months, preserved visual acuity with better quality.
Conclusions
- The application of the Cuban treatment for RP achieves better VA control when performed every 6 months.
- Annual treatment cycles should be evaluated on a case-by-case basis so that control over visual acuity can be achieved.
- Visual acuity control was not achieved if treatment is applied irregularly, outside of the semiannual and annual cycles.
References
- Marc RE, Jones BW, Watt CB, Strettoi E. (2003). Neural Remodeling in Retinal Degeneration. Prog Retin Eye Res. 22(5): 607-55.
- Marc RE, Jones BW. (2005). Retinal remodeling in inherited photoreceptor degenerations. Molecular Neurobiology. 28(2): 139- 47.
- Jones BW, Pfeiffer RL, Ferrell WD, Watt CB, Marmor M, Marc RE, (2016a). Retinal remodeling in human retinitis pigmentosa. Exp. Eye Res 150, 149-165.
- Pfeiffer RL, Marc RE, Jones BW. (2020). Persistent remodeling and neurodegeneration in late-stage retinal degeneration, Prog Retin Eye Res Volume 74, January, 100771.
- Dagnelie G. (2008). Psychophysical evaluation for visual prosthesis. Annu RevBiomed Eng. 10: 339-368.
- The ogarajan LS. (2008). A Low-Power Fully Implantable 15- Channel Retinal Stimulator Chip. IEEE. J. Solid-State Circuits. 43 (10): 2322-2337.
- Zarbin MA, Montemagno C, Leary JF, Ritch R. (2012). Regenerative nanomedicine and the treatment of degenerative retinal diseases. Wiley Interdisciplinary Reviews: Nanomedicine and Nanobiotechnology. Jan; 4(1): 113-137.
- Buchholz DE, Hikita ST, Rowland TJ, Friedrich AM, Hinman CR, Jhohnson LV, et al. (2009). Derivation of functional retinal pigmented epithelium from induced pluripotent stem cells. Stem Cells. 27(10): 2427-2434.
- Enzmann V, Yolku E, Kaplan HJ, IIdstad ST. (2009). Stem cells as a tool in regenerative therapy for retinal regeneration. Arch Ophthalmol. 127(4): 563-571.
- Cai X, Conley SM, Naash MI. (2009). RPE65: role in the visual cycle, human retinal disease, and gene therapy. Ophthalmic Genetics. 30(2): 57-62.
- Pérez Aguiar LJ, García Báez O. (2009). Cuban strategy for the treatment of retinitis pigmentosa. Rev Cubana Oftalmol. [cited 3/04/2013]; 22 (Suppl 2): [approx. 15 p.].
- Peláez Molina O. (1997). Retinitis pigmentosa: the Cuban experience. 1st ed. Havana: Editorial Científico Técnica.
- Pérez LJ, García O, Román C, Menéndez S. (2010). Ozone therapy and electrostimulation in retinitis pigmentosa. Rev. cubana Oftalmol. [cited 11/01/2013]; 23(1).
- Parmeggiani F. (2011). Clinics, Epidemiology and Genetics of Retinitis Pigmentosa. Current Genomics. 12(4): 236-237.
Citation: Perez Aguiar LJ, Herrera Mora M.S, Barrientos Castano A, Herrera Mora M.S and Barrientos Castaño A. (2023). Evaluation of Visual Acuity following Cuban Treatment for Retinitis Pigmentosa. Journal of Ophthalmology and Vision Research 5(1).
Copyright: © 2023 Lázaro Joaquín Perez Aguiar. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.